A new drug that specifically targets cancer cells has shown promising results in phase three clinical trials.
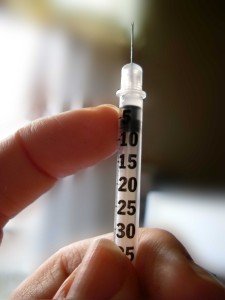
A genetically-modified herpes virus injected into tumours of melanoma patients stimulated an immune response to attack cancer cells, according to research published in the Journal of Clinical Oncology.
The virus replicated inside the cancer cells and used the body’s own immune system to treat the cancer, explained Professor Kevin Harrington, of the Institute of Cancer Research.
“There is increasing excitement over the use of viral treatments like T-VEC for cancer, because they can launch a two-pronged attack on tumours – both killing cancer cells directly and marshalling the immune system against them. And because viral treatment can target cancer cells specifically, it tends to have fewer side-effects than traditional chemotherapy or some of the other new immunotherapies.”
The published results indicated there was improved survival rates of melanoma patients when treated with Talimogene laherparepvec, living on average an extra 20 months compared to the control group.
Our colleagues at the UK Science Media Centre have gathered the following expert commentary on the research.
Prof Dorothy Bennett, Head of the Molecular Cell Sciences Research Centre and Professor of Cell Biology, St George’s, University of London, comments:
“There is currently quite a bewildering array of ongoing trials of new therapies and combinations of new and/or old therapies for malignant melanoma (the most dangerous type of skin cancer).
“This paper reports a trial of another new agent, a herpes virus carrying a gene for the protein GM-CSF, which can stimulate the immune system to attack the cancer. The virus is designed to infect cancer cells and cause them to make GM-CSF, but is modified so that it does not reproduce and infect more cells, nor cause any disease itself. Significant benefit to patients is reported.
“The question many oncologists would ask is, how does this therapy compare with the other new melanoma immunotherapies such as anti-PD1 and anti-CTLA4 antibodies? Or with the new small-molecule agents such as BRAF and MEK inhibitors?
“However this question cannot be answered, because this agent was tested in a specific subset of patients “with less advanced cancers” as the press release puts it. They had to have melanoma nodules amenable to injection, and there was a limit on the number and type of other melanoma nodules around the body. The effects of the other mentioned therapies on this set of patients have not been assessed. Instead, the researchers compared the virus treatment to injections of GM-CSF itself, known to have rather little benefit.
“Moreover the trial was open-label rather than single or double-blind, leading to possible loss of objectivity.
“Overall the findings seem interesting but not earth-shattering, in the context of current therapies for melanoma. However there may well be future value in testing this type of agent in combination with other therapies, as a qualitatively new approach.”
Prof Leonard Seymour, Professor of Gene Therapies, University of Oxford, comments:
“This T-Vec study shows powerful stimulus of an anticancer immune response in patients with melanoma skin cancer. Increasingly we understand that cancer is characterised by suppression of the immune system within tumour deposits, meaning that cancer vaccines have struggled to create useful responses. However T-Vec appears to be able to overcome this suppression within the injected tumour masses and mediates stimulation of an effective anticancer response. There is also evidence of significant tumour shrinkage in 15% of evaluable (non-injected) tumour masses, suggesting a level of systemic immunisation for this type of cancer.
“The next step will be to develop oncolytic virus vaccines that can be given intravenously to reach all metastatic tumour deposits, allowing the same vaccine effects in all tumour growths – at this stage it’s very promising that this appears to have positive results for melanoma skin cancer, but we need further research to see whether it could be relevant to other cancers too.
“This study represents a culmination of many years of research into oncolytic viruses as cancer-specific therapeutics. Oncolytic viruses combine four crucial advances compared to conventional cancer treatments:
1. They amplify themselves selectively within tumour cells, increasing the amount of therapeutic agent locally without causing high levels in the bloodstream. This maximises anticancer activity and minimises unwanted side effects.
2. Their selectivity for cancer cells depends on the cancer phenotype and can be far more selective than traditional chemotherapy agents that merely target cells that are proliferating.
3. Oncolytic viruses can kill cells actively (not always dependent on cellular pathways of apoptosis), providing the possibility of a more inflammatory death pathway that can be used to produce a cancer vaccine.
4. They can encode biologics for expression selectivity within the tumour (in this case a molecule called GM CSF). This provides a whole new approach to using novel biological therapeutics that are often too toxic to be given to patients as proteins, but should be very effective when produced by the patient’s own tumour cells in situ.
“The oncolytic virus field has been buzzing in recent years, with hundreds of scientists involved worldwide, and the next international event will be held in Boston in two weeks’ time (http://ovcboston.com/).
“Oncolytic virus vaccines should synergise perfectly with the other big recent advance in cancer therapy – ‘immune checkpoint inhibitors’. Whereas oncolytic vaccines can stimulate an anticancer immune response, checkpoint inhibitors potentiate the ability of the immune system to respond. The combination of T-Vec with anti-CTLA4 has already shown astonishing results (Puzanov et al., http://meetinglibrary.asco.org/content/128142-144).”
Declared interests
Prof Dorothy Bennett: “I declare no conflict of interest.”
Prof Leonard Seymour: “I am Professor of Gene Therapies at the University of Oxford, specialising in oncolytic viruses. I have about 15 years’ experience in this field. I declare an interest, as a founding scientist and consultant for PsiOxus Ltd, which is developing oncolytic vaccines for intravenous delivery rather than direct intratumoral injection.”