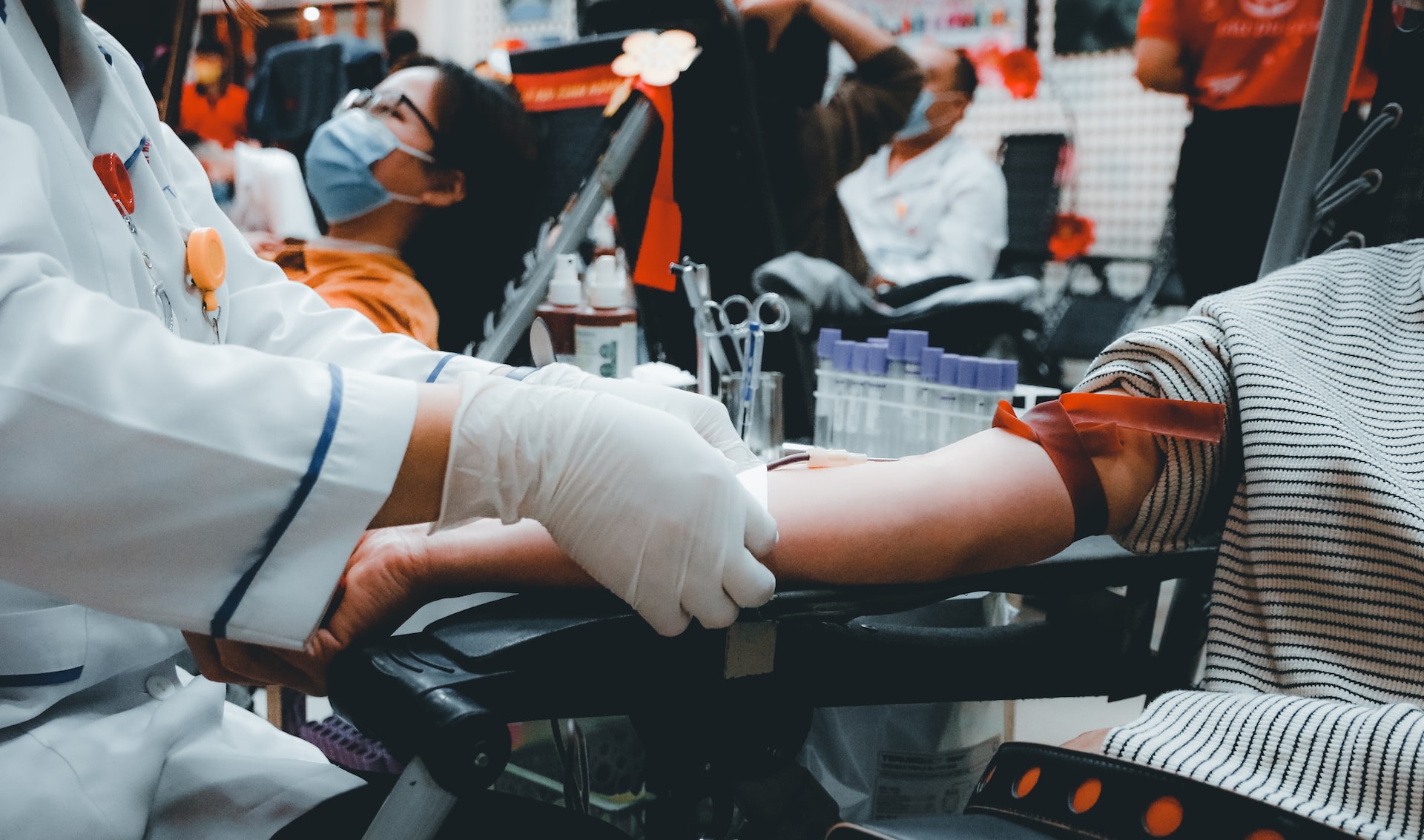
The parents of a baby who needs life-saving open heart surgery are insisting that ‘the bulk’ of his blood transfusion comes from donors who haven’t had the COVID-19 vaccine.
Te Whatu Ora Health New Zealand wants the courts to take temporary custody of the four-month-old baby so that he can have open-heart surgery using blood from the NZ Blood Service which may have come from donors vaccinated against the Covid-19 virus. A full hearing will be held on Tuesday in the High Court at Auckland.
The SMC asked experts to explain the science behind New Zealand’s blood transfusion procedures and policies, and how the Pfizer vaccine interacts with our blood.
Dr Jim Faed, Senior Lecturer, Haematologist and Transfusion Medicine Specialist, Department of Pathology (Dunedin), University of Otago, comments:
When is direct blood donation allowed in New Zealand?
“‘Directed blood donations’ are blood donations that are arranged by an individual, family or group of people for a named person; i.e. the blood donations are directed to the named person. Directed blood donations are rare in NZ. Most requests for directed donations have come from parents who wanted to provide blood for their newborn baby or infant before surgery or some other health procedure. In the past, most requests have arisen from anxieties over the risk for HIV infection in the 1980s-90s and hepatitis C in the 1990s. However, when the risks of being infected by one of these viruses by a transfusion in NZ are explained, most accept that the risks are much smaller than imagined. Most parents have then accepted a transfusion of blood components provided by the Blood Service.
“However, a reserve stock of blood components is always needed in case a patient’s requirements are greater than anticipated. If a reserve stock of blood is collected for a named person, the ‘directed’ patient, and is not used for that patient, the blood cannot be transferred to the general blood component stocks.
“The issue for NZ Blood Service is likely to be – who pays for the service of setting up the arrangements and the cost of any blood or blood components that are not transfused? The Blood Service does not receive a funding grant from the Government. It is funded by charges to Public Hospitals for the cost of collecting, testing, processing, and supplying blood components and products transfused in their region.
“In addition, directed donations will not be available if a surgery date for a patient is changed to a later date and some or all of the items directed have expired or are no longer suitable. Changes to surgery dates are common if hospitals are overloaded and patients are admitted with acute conditions and occupy the surgery beds.
“Who will pay for the ‘directed blood’ that is not transfused? It is usual to have a buffer stock of extra blood components available in case unexpected surgery problems arise and more blood is needed. An extra buffer stock is easily managed in a volunteer blood donor and donation system. If not used for one patient the stock is held for the next patient. That will not happen for a ‘directed donation’ as it can only be used for one individual. Currently, there is no system in existence to charge for unused blood. NZ law prevents charging patients directly for blood and blood components used for health treatments. The law does not envisage a system where ‘directed donations’ are not used.
“Finally, the reserve stocks of special blood components – plasma, platelets and cryoprecipitate are always available from truly volunteer donors. These are separate production and supply lines for whole blood and red cells. They are needed for some surgery procedures, such as cardiac and other large surgery procedures and acute trauma patients. No system anywhere in the world, as far as I know, has a ‘directed donor’ system to supply all of these blood components. They are often needed in cardiac surgery, and a need cannot always be anticipated.
“A question to be posed to those who believe that the Covid-19 vaccine will change the safety of blood is whether that applies to all blood components such as red cells, platelets, plasma and cryoprecipitate. A similar question is whether the highly purified processed blood products – Immunoglobulins, Albumin and blood clotting factors are also affected. Answers to these questions are important as they will affect health treatments for many people.”
Why isn’t it recommended?
“Directed donation is not recommended for many reasons, but the most important one for the recipient is the concern over safety. The safety of blood is a continuing focus for all Blood Services. Requests for directed blood donations raise additional safety issues. They arise because the ‘directed donors’ may consider themselves in good health and then decide they are safe to give blood. When they come to answer the blood donor questionnaire and the verbal questions in the standardised donor screening process, a person may be tempted to answer ‘no’ – this does not apply to me, instead of ‘yes’ – it does or could apply to me. People being screened before being accepted as a ‘directed donor’ may be tempted to give answers that will ensure they can give blood on that day. Failing to give the true (correct) answer will create a risk for the person who may receive a transfusion from that potential ‘directed donor’. Directed donations are therefore regarded as being less safe from infection and other risks by Blood Transfusion Specialists.
“The Blood Service and Blood Banks in Hospitals are required to store directed donations separately from volunteer blood stocks as the directed items do not meet the requirements for blood donor screening, and some may have a higher risk for infectious agents. Directed blood donations are also kept separate so that they can be readily identified and sent to the appropriate Blood Bank for the planned surgery date. Separate storage is also required so that directed donations are not inadvertently given to other patients. Where humans are required to use manual systems to store multiple items separately, mistakes can occur. Probably the greatest risk is that a voluntary donor blood component may be supplied instead of a directed donation. The reverse is highly unlikely.
“Issues of physical space availability arise in Hospital Blood Banks. If more than one person makes a directed donation request in a region, the issue will rapidly become unmanageable for the local Hospital. Additional temperature-controlled storage facilities would be needed to keep the directed blood donations separate from volunteer blood and as separate lots for each directed patient. The refrigeration required is specialised, must run at specific temperatures and be monitored with a complete record of temperatures; it is not a simple matter of popping down the road and buying another fridge. Many Blood Banks have limited space and cannot accommodate extra temperature-controlled storage facilities. I am not aware of anyone attempting to set up such a system anywhere in the world.
“Although the term blood transfusion is here to stay, whole blood is rarely transfused in modern hospitals. Most hospital transfusions are given as blood components – red cells, plasma, platelets or cryoprecipitate. Occasionally a mix of several blood components is given in the proportions needed by an individual patient. Complex surgery procedures such as heart surgery often require specialised blood components such as plasma, platelets and cryoprecipitate. Blood components are used to stop or prevent bleeding from various causes and, if needed, to replace red cells if anaemia is a problem. Transfusing blood components is the safest and most cost-effective way to provide for the transfusion needs of hospital patients. Blood components are obtained by the Blood Service from the blood donations given by volunteer donors. Some blood components require selected donors identified by the Blood Service as meeting the additional criteria. Whole blood is often used during cardiac surgery procedures on babies and small children, and may be given to some people with severe bleeding after trauma.
“When ‘directed donations’ are requested, it would be very difficult to plan to have directed blood components for a surgical procedure. A patient undergoing cardiac surgery may need one or more of these specialised blood components at the end of surgery to stop bleeding. Platelets have a high cost of collection, testing and supply, and the current approved price for Hospitals is greater than $800 for each item. The Blood Service is most unlikely to be willing to collect platelets from directed donors and have the platelets available on a just-in-case basis. Health issues would arise for an inexperienced donor.
“Ultimately, there are no shortcuts to safety! That is why the Blood Service exists as a separate entity from the Hospitals and other Healthcare providers – to achieve the required levels of safety.”
Conflict of interest statement: “I am not employed by the NZ Blood Service (NZBS). I was involved from 1982-2020 in developing policies and operating standards used in New Zealand, first in the Regional Blood Services until 1998 when the NZBS was established, and then in the NZBS as a Transfusion Medicine Specialist.”
Immunisation Advisory Centre, University of Auckland, comments:
Is the COVID-19 vaccine safe?
“The Comirnaty (Pfizer) vaccine has been extensively used internationally and shown to have an excellent safety profile. For example Vaccine safety monitoring of mRNA vaccines for the first 6 months of the USA rollout included more than 298 million doses administered. The safety monitoring on this was noted to be “the most comprehensive of any vaccine in US history”. This established an excellent safety profile. This data is further supported by international meta-analysis which reviews multiple publications on safety data, confirming the excellent safety profile.
“The vaccine has known short term reactions including injection site pain, redness and swelling as well as systemic reactions such as fatigue, headache, muscle aches, chills and fever. These are most often mild and resolve in 1 to 2 days. Lymphadenopathy (swollen lymph nodes) may also occur. The safety has been carefully scrutinised in the real world and in addition to the known reactions already mentioned the risk of anaphylaxis and myopericarditis rates are increased. Anaphylaxis may occur after any vaccination and is able to be managed by vaccination centres. The myopericarditis is generally mild but can have serious outcomes if not addressed. The rate of myopericarditis is higher after COVID infection than after the vaccination.
“While the viral vector-based vaccines produced by AstraZeneca and Janssen are both associated with thrombotic events, the Pfizer vaccine (mRNA) used in New Zealand has not. These are different vaccines. Numerous studies including one performed in New Zealand have not found an increased risk of cardiovascular events due to clots with the Pfizer vaccine.
“There are numerous safety reports from our country, UK, Australia, Canada, USA and European
countries. The Medsafe Updated summary of risk management plan for Comirnaty (COVID-19 mRNA
vaccine) is an example of the close scrutiny being applied to the vaccine. In it Medsafe lists the
known risks (anaphylaxis, myocarditis, pericarditis) as well as potential risks.”
Can the products of the COVID-19 vaccine end up in the blood stream?
“Spike protein is the protein on the surface of SARS-CoV- 2 virus; the shape it forms gives coronaviruses their name (corona = crown). It is used by the virus to attach to cells in the airways to infect them and to spread from cell to cell. The SARSCoV-2 virus contains RNA that gives the body instructions to make new virus including virus spike proteins. These spread throughout the body during infection. Our body only makes these spike proteins when we are infected with SARS-CoV-2, or vaccinated with the mRNA code.
“The quantity of this spike protein produced after vaccination is much lower than the amount seen in people with COVID-19 infection with the virus spreading throughout their body. Furthermore, as soon as it is produced, this protein is dismantled inside specialist cells and the pieces are shown to the immune system in the lymph nodes nearest to the arm muscle when the vaccine was delivered. Research shows that most of the vaccine product stays in the muscle, local lymph node and a small amount may travel to the liver (where all waste products are taken).
“Very low levels of spike protein (mean peak level 86 pg/ml) have been detected in plasma of people vaccinated for the first time with another mRNA vaccine (Moderna vaccine). This vaccine contains twice as much RNA as the Pfizer vaccine used in New Zealand. Spike protein was detected as early as day 1 after vaccination, peaked on average 5 days after vaccination and declined and became undetectable by day 14 in all participants. No spike protein was detectable after the second vaccine dose.
“The quantity of this protein produced after vaccination is much lower than the amount seen in people with COVID-19 infection, where the virus spreads throughout their body. No harm from antibodies from the Comirnaty vaccine being present in the blood stream. There is no evidence of harm from antibodies being present in blood, which are produced in response to both natural infection and vaccination. Although unlikely to be present in blood products, any components or products of the vaccine that may potentially be present in blood (lipid nanoparticles, mRNA or the spike protein) would not be harmful if they were to be transferred through blood transfusion.”
Is there a concern about lipid coat in the vaccine?
“The low amount of vaccine product in a single dose limits the distribution of the RNA and lipid nanoparticles mainly to the injection site and to migrating antigen-presenting cells. Due to the transient expression of the RNA, no persistent expression is expected. The lipids used in the nanoparticles, including cholesterol, are mostly normal products in the body or in our foods and medicines, and are processed in the liver.”
Are there risk factors with donor blood?
“There are known risks associated with transfusions from donor blood such as an allergic reaction, or the receiver of the blood becomes infected with a virus if the blood has not been effectively screened. This is not related to the COVID vaccination status of a donor. Although unlikely to be present in blood products, any components or products of the vaccine (nanoparticles, mRNA or the spike protein) would not be harmful if they were to be transferred through blood transfusion.
“Detecting mRNA in blood is unlikely. The mRNA is only very briefly in a person’s body (mainly in the muscle and nearby lymph nodes) after vaccination before being broken down by widespread enzymes. It is unlikely there is any detectable mRNA in the small volume of a person’s blood that is given when donating blood. There has been no recorded international concerns with use of donor blood from COVID vaccinated donors, and COVID vaccines have been used extensively internationally.”
“Once outside of its lipid bubble, mRNA is quickly destroyed by enzymes (ribonucleases) found everywhere, including inside and outside of our cells. It only has a day or two to do its work. The mRNA is transiently expressed, does not integrate into the genome and is degraded by physiological pathways- there are numerous enzymes present in our cells for this. The components of the lipid bubble are also cleared from our body as a waste product. The quantity of this spike protein produced after vaccination is much lower than the amount seen in people with COVID-19 infection with the virus spreading throughout their body. Furthermore, as soon as it is produced, this protein is dismantled inside specialist cells and the pieces are shown to the immune system in the lymph nodes nearest to the arm muscle. Given these facts, checking the presence of spike protein, and then distinguishing if the spike protein has been produced in response to either vaccine or virus, would be very difficult and have no clinical purpose.”
No conflict of interest declared